Deep Vein Thrombosis (DVT): Symptoms and Prevention
Learn the symptoms, causes, and prevention of deep vein thrombosis (DVT) and when to seek medical care to avoid serious complications.
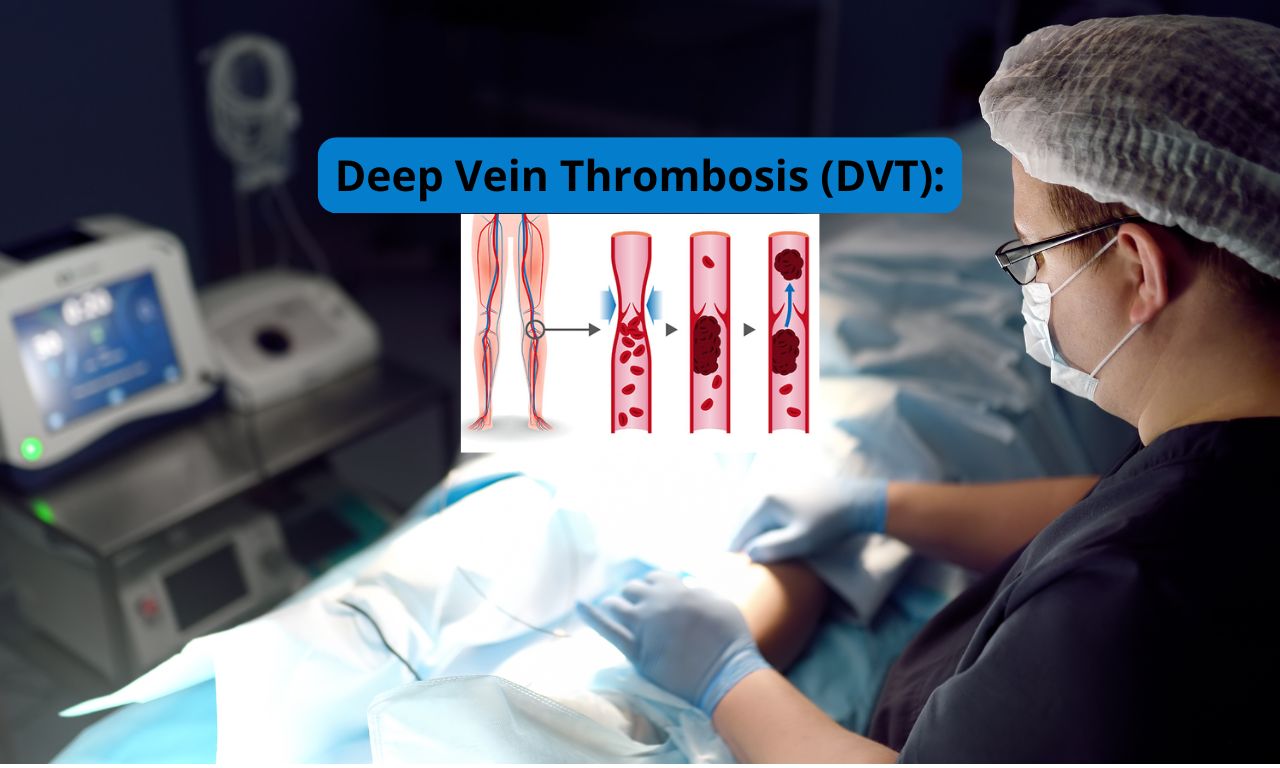
Deep Vein Thrombosis (DVT) is a serious vascular condition that occurs when a blood clot forms in a deep vein, most commonly in the legs. While some cases may cause noticeable symptoms, others may develop silently, making early detection and prevention critically important.
If left untreated, DVT can lead to potentially life-threatening complications such as pulmonary embolism, a condition in which a blood clot travels to the lungs and blocks blood flow.
Understanding the warning signs, causes, and prevention strategies for deep vein thrombosis can help patients reduce their risk and seek timely medical care.
What Is Deep Vein Thrombosis?
Deep Vein Thrombosis occurs when a blood clot (thrombus) forms in one of the deep veins of the body. These veins are typically located deep within the muscles of the legs, although DVT can also occur in the arms or pelvis.
Blood clots develop when the normal flow of blood slows or when the blood becomes more likely to clot.
This condition is often associated with Virchow’s Triad, a combination of three factors that contribute to clot formation:
- Reduced blood flow (venous stasis)
- Damage to the vein wall
- Increased blood clotting tendency
When a clot forms in a deep vein, it can partially or completely block blood flow.
The greatest concern occurs if part of the clot breaks free and travels through the bloodstream to the lungs, causing a pulmonary embolism (PE).
Causes and Risk Factors
Several medical conditions and lifestyle factors can increase the risk of developing deep vein thrombosis.
Prolonged Immobility
Long periods of inactivity can slow blood circulation in the legs.
Examples include:
- Long airplane flights
- Extended car travel
- Bed rest after surgery
- Hospitalization
Surgery or Injury
Major surgery—particularly orthopedic procedures involving the hips or knees—can increase the risk of blood clot formation.
Pregnancy
Pregnancy increases pressure in pelvic veins and alters the body’s clotting mechanisms.
Hormonal Medications
Certain medications may increase clotting risk, including:
- Birth control pills
- Hormone replacement therapy
Medical Conditions
Certain medical conditions may increase clot risk, such as:
- Cancer
- Heart disease
- Obesity
- Genetic clotting disorders
Previous Blood Clots
Individuals with a history of DVT or pulmonary embolism have a higher risk of recurrence.
Symptoms and Warning Signs
In some cases, DVT may cause minimal or no symptoms. However, when symptoms occur, they typically affect one leg.
Common warning signs include:
- Swelling in one leg
- Pain or tenderness in the calf
- Warmth in the affected area
- Red or discolored skin
- Leg heaviness
Symptoms may worsen when standing or walking.
If a pulmonary embolism develops, symptoms may include:
- Sudden shortness of breath
- Chest pain
- Rapid heartbeat
- Coughing up blood
Pulmonary embolism is a medical emergency that requires immediate treatment.
Diagnosis and Medical Evaluation
Early diagnosis of deep vein thrombosis is essential to prevent complications.
Physicians typically begin with a clinical assessment and evaluation of risk factors.
Common diagnostic tests include:
Duplex Ultrasound
The primary imaging test used to detect blood clots in the veins. Ultrasound can visualize the clot and assess blood flow.
D-Dimer Blood Test
This blood test measures substances released when a clot dissolves. Elevated levels may indicate the presence of abnormal clotting.
Advanced Imaging
In some cases, physicians may use additional imaging such as:
- CT venography
- MRI venography
These tests provide detailed visualization of the venous system.


Treatment Options
Treatment of deep vein thrombosis focuses on preventing the clot from growing and reducing the risk of pulmonary embolism.
Anticoagulant Medications
The most common treatment involves blood-thinning medications, also known as anticoagulants.
These medications help prevent new clots from forming and reduce the risk of complications.
Common anticoagulants include:
- Heparin
- Low molecular weight heparin
- Direct oral anticoagulants (DOACs)
Compression Therapy
Compression stockings may help reduce swelling and improve blood circulation.
They may also reduce the risk of post-thrombotic syndrome, a long-term complication of DVT.
Thrombolytic Therapy
In severe cases, medications that dissolve clots may be used.
These treatments are typically reserved for large or life-threatening clots.
Interventional Procedures
Some patients may require specialized procedures, such as:
- Catheter-directed thrombolysis
- Mechanical thrombectomy
- Placement of an inferior vena cava (IVC) filter
These interventions are used in specific high-risk situations.
Prevention and Lifestyle Recommendations
Preventing deep vein thrombosis is particularly important for individuals at higher risk.
Recommended prevention strategies include:
- Regular physical activity
- Avoiding long periods of immobility
- Walking during long flights or road trips
- Staying hydrated
- Maintaining a healthy weight
For high-risk patients, physicians may recommend preventive anticoagulation therapy during periods of increased risk, such as after surgery.
Compression stockings may also be recommended in certain cases.
When to See a Vein Specialist
Patients should seek medical evaluation immediately if they experience symptoms such as:
- Sudden swelling in one leg
- Persistent calf pain
- Unexplained redness or warmth in the leg
Emergency medical attention is required if symptoms of pulmonary embolism occur, including sudden shortness of breath or chest pain.
Early diagnosis and treatment significantly reduce the risk of serious complications.
Frequently Asked Questions (FAQ)
Is deep vein thrombosis dangerous?
Yes. DVT can become life-threatening if the clot travels to the lungs and causes pulmonary embolism.
How long does treatment last?
Anticoagulant therapy typically lasts three to six months, although some patients may require longer treatment.
Can DVT occur without symptoms?
Yes. Some patients develop DVT with few or no symptoms, which is why risk assessment and prevention are important.
Who is most at risk for DVT?
Individuals with prolonged immobility, recent surgery, cancer, pregnancy, or previous blood clots have a higher risk.
Can deep vein thrombosis be prevented?
In many cases, yes. Staying active, avoiding prolonged sitting, and following medical advice during high-risk situations can reduce the risk.
Medical Credibility (autor)
Medically reviewed by
Dr. Alejandro Cabrera
Specialist in Phlebology and Vascular Medicine